Docs Call in the Cops
And other strategies for treating agitated patients
Take a look at this video when you’ve got time.
It’s a hospital situation any one of us could face.
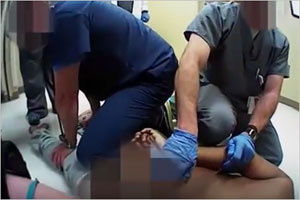
The body camera footage, publicly available on YouTube, was released by police. It’s of an incident at Athens-Limestone Hospital, Alabama, where 49-year-old Randy Joe Nelson was stunned with a Taser. He died five days later.
Treating an agitated patient who may, or may not, pose a risk of harm to staff—and having a strategy for when to call in the police—have been subjects under discussion by members of ACLP’s Emergency Psychiatry Special Interest Group (SIG).
Although much research has been dedicated to the management of delirious agitation, consulting psychiatrists must also diagnose and manage agitation secondary to intoxication, personality disorders, instrumental aggression, or unclear pathologies.
For many of these situations, the appropriate treatment remains a dilemma—controversial and subject to opposing recommendations and evidence.
Should ketamine or antipsychotics and benzodiazepines be used for agitation with abnormal vital signs?
Agitation presenting with tachycardia, hypertension, and/or fever raises concern for excited delirium. Ketamine is increasingly administered for symptom control in these presentations, although benzodiazepines and antipsychotics continue to have utility.
Should haloperidol or atypical antipsychotics be used for agitation with alcohol intoxication?
Haloperidol has been recommended as the first line treatment for agitation from alcohol intoxication. Even so, the evidence base of its use in these situations is sparse, and alternative agents are commonly used despite risks of adverse effects from atypical antipsychotics and benzodiazepines.
Do medications have a role in agitation in developmental delay?
Patients with developmental delay may be challenged by the stressful and stimulating health care environment. Moreover, these patients may be challenged to engage in traditional verbal de-escalation. Emergency departments should keep a “comfort cart” or cabinet from which patients can select distracting and calming activities; online websites sell such toys ideal for children and adults with intellectual disabilities. In studies, as many as 73% of children with these disabilities are prone to adverse effects from medications.
Should benzodiazepines or antipsychotics be used for agitation with stimulant intoxication?
Antipsychotics remain widely used for cocaine, methamphetamine, and PCP intoxication, even though benzodiazepines have been recommended as the first line treatment. That psychosis secondary to primary psychiatric illness is indistinguishable from that induced by substances complicates medication selection.
Agitation assessment practice
Regardless of etiology, there is broad agreement that all agitation should be initially approached in the same manner. Agitation should be assessed with an objective clinical scale, such as the Richardson Agitation Sedation Scale. And all staff, including security, should be trained in verbal de-escalation techniques and attempt to verbally de-escalate the agitated patient before administering medications.
Tips for verbal de-escalation, from the American Association for Emergency Psychiatry, urge clinicians to:
- Respect personal space.
- Avoid provocation.
- Establish verbal contact.
- Be concise.
- Identify wants and feelings.
- Listen closely to what the patient is saying.
- Agree, or agree to disagree.
- Set clear limitations.
- Provide choices and optimism.
Scott Simpson, MD, MPH, co-chair of ACLP’s Emergency Psychiatry SIG, has published with his colleagues at Denver Health Medical Center an online video series teaching these, and more advanced, skills for students and trainees.
When medication is necessary, he says, oral medication should be preferred over intramuscular or intravenous agents, and seclusion or restraint should be avoided if at all possible, subject to risks to the patient and staff.
But when do you resort to calling in the police? And can clinicians influence law enforcement techniques?
In the video of Randy Joe Nelson, he was reportedly brought to the hospital by family who were concerned that symptoms of his bipolar disorder had worsened. When the SIG’s members first highlighted the video at ACLP’s annual conference last fall, however, they questioned whether (in February 2016 when the incident happened) the hospital had a collaboration strategy in place with local police for dealing with such events.
Evolving collaboration strategies in the hospital
Security personnel have operated in hospitals since the 1950s. By the 1980s, safety measures were switched from primarily reactive to proactive, i.e.: prevention and, in more recent decades, they became integrated into electronic security with a focus on risk management.
In-house hospital security officers aim to prevent incidents, protect the organization, and administer remedies through strategies defined by the hospital. They help care for violent or uncooperative patients; disarm them if they are carrying weapons; and seek to defuse tense or escalating situations.
By comparison, the role of external law enforcement officers has primarily been to apprehend offenders (to protect society) and use legal remedies defined by statute. Their role is to protect victims and escort patients into custody.
Research suggests there is as much controversy in deploying security as there is in prescribing treatment.
Some emergency department clinicians expect the worse when they see either internal security or external law enforcement officers—and fear their “hard” uniforms may escalate violence and diffuse trust. Some patients and families also perceive uniformed officers to be antagonising. That, in turn, has led to “undercover” security officers operating in “soft” uniforms, to date in approximately 12% of US hospitals.
But, others say optimal care for patients can be achieved only when the emergency department is secure against violent acts and security. Thus, both internal security and external law enforcement are significant parts of the emergency department workforce. Some patients and visitors also favor their presence to create a safe and secure environment.
Working with law enforcement in the community
The American College of Emergency Physicians’ policy is that, except where legally required, information about a patient should not be released without permission from the patient or surrogate decision-maker and that “law enforcement activities should not interfere with patient care.”
Under the federal 1986 Emergency Medical Treatment and Labor Act, anyone arriving in an emergency department must be stabilized and treated. Hospitals cannot refuse care to agitated or critically ill patients, and a physician must treat them with or without the presence of security or law enforcement officers.
So . . . hospitals—treading the line between in-house security tasked with de-escalation and law enforcement officers tasked with apprehending offenders—have increasingly sought a partnership between hospital security staff and local police, and seek to influence law enforcement policies in ways that can facilitate collaboration.
A professional organization for those managing security and safety in health care, the International Association for Healthcare Security and Safety, has issued new guidelines on collaborating with law enforcement designed to improve safety and relationships with law enforcement.
Moreover, law enforcement agencies have shown themselves to be highly motivated to improve their processes. The impetus for improved training among law enforcement officers comes from:
- Recognition of challenges faced by officers
- Increase in mental health encounters
- Court decisions on wrongful death and excessive use of force
- Department of Justice regulations
- Practical benefits for police of good community relations
Like that of internal security officers, police officers’ training focuses on verbal de-escalation. The most common model for police training in managing patients with mental illness is Crisis Intervention Training (CIT). Some police departments provide all officers with CIT, although in most cities only specialized “teams” receive CIT. Barriers to training police include the cost of training, differences among police departmental cultures, and the level of interest exhibited among individual officers.
Says Dr. Simpson: “Consulting psychiatrists can be proactive in supporting their local law enforcement agencies to better care for patients with mental illness by:
- Collaborating and consulting through police committees on policy development
- Presenting at law enforcement training sessions
- Establishing co-responders with law enforcement in critical situations
- And . . . proactively seeking to maintain good relationships.”